Interesting Case: October 2018
Case contributed by:
Suntrea Hammer, MD, Assistant Professor, University of Texas Southwestern Medical Center, Dallas, TX
Clinical History
A 41-year-old woman with a history of interstitial lung disease, obesity, and polysubstance abuse presented with mildly, but persistently elevated transaminases (AST 53, ALT 38) and mild thrombocytopenia (113,000/uL).
Imaging
Abdominal ultrasound demonstrated massive hepatosplenomegaly with normal hepatic contours and hepatopetal flow.
Chest CT revealed bilateral upper lobe pulmonary fibrosis concerning for sarcoidosis, infection, or hypersensitivity pneumonitis. There was also pulmonary artery enlargement, consistent with pulmonary arterial hypertension.
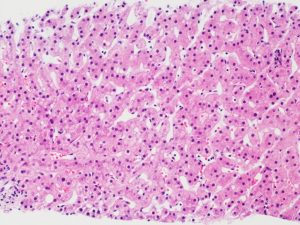 |
| Figure 1: H&E 20x |
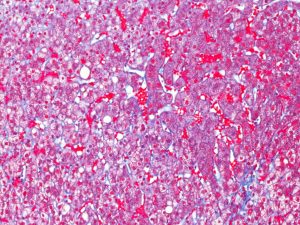 |
| Figure 2: Trichrome 20x |
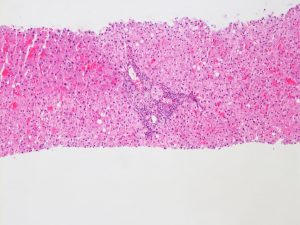 |
| Figure 3: H&E 10x |
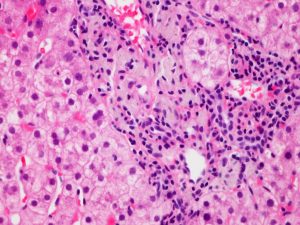 |
| Figure 4: H&E 40x |
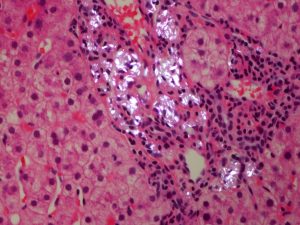 |
| Figure 5: H&E 40x polarized light microscopy |
Liver Biopsy Findings
The liver biopsy has mild central zone and sinusoidal dilatation (Figure 1) with delicate perisinusoidal fibrosis on trichrome stain (Figure 2), consistent with the patient’s history of pulmonary hypertension. There is minimal macrovesicular steatosis and no significant lobular inflammation (Figure 3). The portal tracts are remarkable for a prominent histiocytes with a pale gray, grainy cytoplasm and a wrinkled “tissue paper” appearance (Figure 4). The histiocytes are illuminated on polarization demonstrating polarizable crystalline material (Figure 5).
Diagnosis
Talc related portal histiocytosis in an intravenous drug abuser
Mild congestive hepatopathy secondary to pulmonary hypertension
Major Learning Points
- Talc presents in the liver as polarizable, needle-shaped crystals within portal macrophages. Granulomata are rare, unlike the reactions seen in the lung.
- Talc histiocytosis can present along-side chronic viral hepatitis or congestive hepatopathy in patients with concomitant lung related injuries.
- The presence of talc alone is not reported to lead to chronic liver injury or fibrosis, and the talc may persist long after drug use has ceased.
Discussion
Talc is an insoluble crystal present in many pharmaceuticals as a “filler” substance. When these pharmaceuticals are ground down for intravenous injection, the talc particles are distributed around the body, most commonly in the lung, but also in the liver in as many as 63% of users (1).[i]
Unlike cases of pulmonary deposition, talc deposition in the liver is devoid of giant cells and well-formed granulomas. Typical talc deposits are seen as infiltrates of hypertrophied macrophages with gray cytoplasm and indistinct cytoplasmic crystals within the portal tracts, and occasionally, in Kupffer cells.[ii] These infiltrates can be associated with inflammatory infiltrates and fibrosis, usually in the setting of chronic viral hepatitis. In this case, the patient had talc induced pulmonary fibrosis, which led to pulmonary hypertension and right heart dysfunction, the sequela of which can be identified in the liver as vascular outflow obstruction.
The histologic features of talc induced histiocytosis are subtle and can easily be mistaken for debris laden macrophages. Unlike classic debris laden macrophages, the cytoplasm has a “wrinkled tissue paper” quality, which suggests the presence of cytoplasmic crystals. These differ from the polarizable crystalline deposits in porphyria, which demonstrate a “Maltese cross” pattern.[iii] The cytoplasm in glycogen storage diseases can also take on a “wrinkled tissue paper” quality, but this will be primarily within hepatocytes rather than histiocytes.[iii]
[i] Allaire GS, Goodman ZD, Ishak KG, Rabin L. Talc in liver tissue of intravenous drug abusers with chronic hepatitis. A comparative study. Am J Clin Pathol. 1989 Nov;92(5):583-8.
[ii] Kringsholm B, Christoffersen P. The nature and the occurrence of birefringent material in different organs in fatal drug addiction. Forensic Sci Int. 1987 May-Jun;34(1-2):53-62.
[iii] Burt A, Portmann B, Ferrell L. MacSween’s Pathology of the Liver. 6th edition. Churchill Livingston Elsevier; 2012. Chapter 4, Genetic and Metabolic Diseases.
